Diabetic Exams & Treatment are Available in all Locations
Mount Vernon (Little Mountain Lane and Market Street), Sedro Woolley, Stanwood & Coupeville


Diabetic retinopathy is a deleterious effect of diabetes on the eyes. People with diabetes are at risk of developing this retinal disease, which can ultimately lead to blindness if left untreated. Diabetic retinopathy can be treated or prevented with lifestyle changes, medication or laser procedures if detected early. The symptoms of diabetic retinopathy will not become evident until permanent damage has already been done, so early detection is key. Diabetics can also be at a higher risk of developing cataracts. These annual dilated eye exams, even if vision appears to be fine, are the best way to monitor retinal health and cataracts to prevent permanent changes to vision.
If you are being examined for an eyeglass or contact lens prescription during your appointment, it is important to have the examination when your blood sugar is stable. Fluctuations in blood sugar can cause changes in your glasses prescription, so it is best to keep your blood sugar balanced for several days prior to your visit.
Who is at risk?
For any type of diabetes, there are two main risk factors for retinopathy: duration of the diabetes disease and how well blood sugar is controlled. Smoking and high blood pressure can also increase your risk. People who have had Type I diabetes for at least ten years have a higher risk of developing diabetic retinopathy. Anyone who has Type II diabetes or borderline diabetes (“pre-diabetic”) should be seen for a baseline exam soon after the initial diagnosis, since signs and symptoms will not be noticeable until permanent damage has already occurred and retinopathy may be present at the first time of diagnosis. Eye exams should be performed on a yearly basis for any type of diabetes.
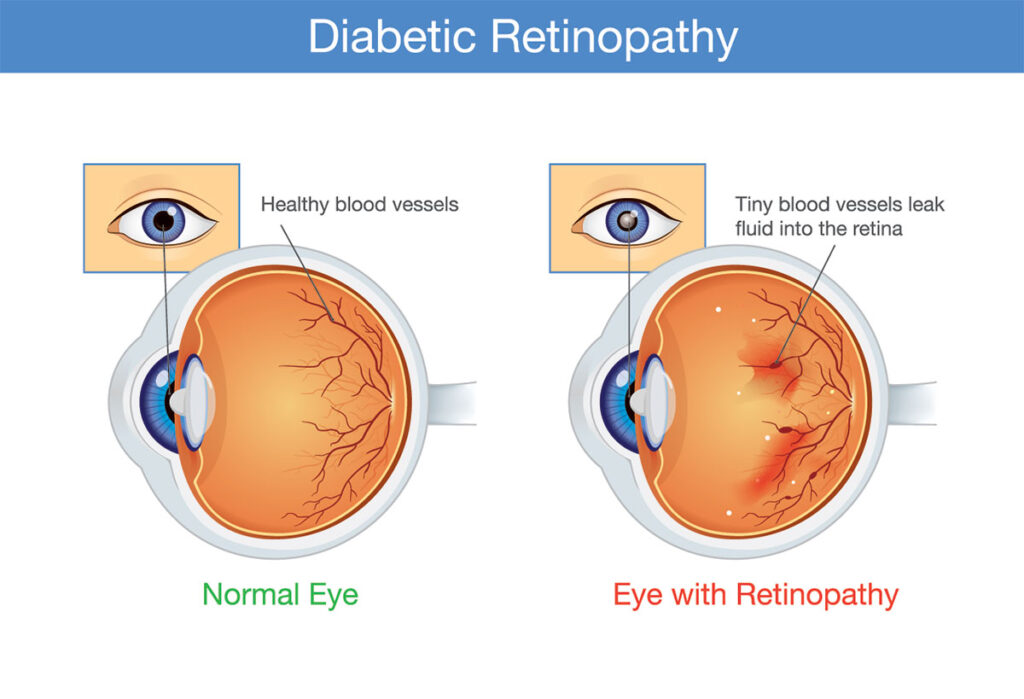
How does diabetes affect my eye?
When blood sugar levels are high, they can cause damage to vessels in the retina. This damage may cause leaking of serum that can accumulate in the center of the retina (called the macula). The result is “macular edema,” and it can reduce your ability to see fine details. If the disease progresses, abnormal vessels can develop on the surface of the retina. These vessels can also bleed or create scar tissue, leading to worsening eyesight, retinal detachments, and eventually a complete loss of vision.
Signs of diabetic retinopathy
Potential signs of diabetic retinopathy include:
- Hazy vision
- “Floaters”
- Missing spots of vision
- Double vision
If you have noticed some or all of these symptoms, please contact us as soon as possible to make an appointment. We will diagnose the issue and move forward with an appropriate treatment plan in order to help prevent future damage and preserve your remaining vision.
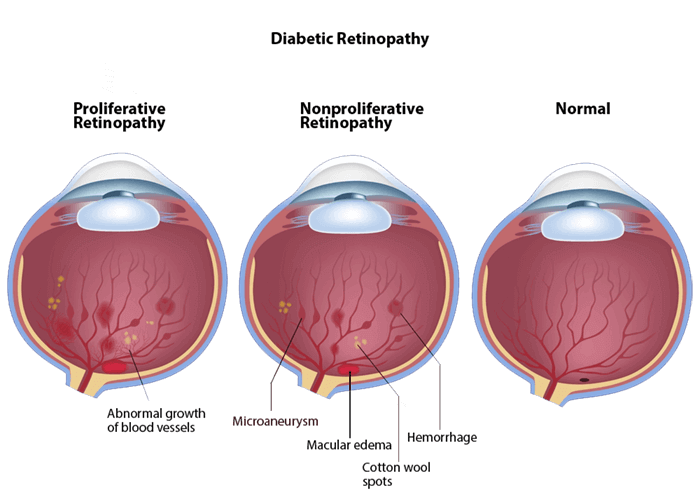
Stages of Diabetic Retinopathy
There are two main categories of diabetic retinopathy: non-proliferative diabetic retinopathy (NPDR) and proliferative diabetic retinopathy (PDR).
NPDR is the early stage of diabetic retinopathy, which affects more people overall. Diabetes gradually causes the blood vessels to get weaker and leak some fluid into the retina. Excess fluid in the retina then starts to downgrade vision.
PDR is the more advanced stage of this condition. This occurs when damage to the blood vessels becomes so severe that the patient’s body starts to create new, faulty blood vessels to take their place. Unfortunately, these vessels are very likely to leak, exacerbating the problem by creating scar tissue that can damage the retina and the optic nerve.
Although one in three patients over the age of 40 with diabetes develops diabetic retinopathy, the good news is that you can prevent this condition from developing (or becoming more serious) by managing your blood sugar and seeking treatment.
Diabetic Retinopathy Diagnosis
Since early diabetic retinopathy symptoms are minor, all patients with diabetes should undergo regular comprehensive eye exams to keep tabs on their eye health before suffering permanent vision loss.
Our doctors check for diabetic retinopathy with a dilation test. Once the patient’s pupils are dilated, the doctor can see the back of the eye more clearly and look for any worrisome abnormalities like new blood vessels, blood in the vitreous, scar tissue on the retina, or damage to the optic nerve.
If the doctor does notice signs, he or she may administer further tests like an OCT (optical coherence tomography) that generates a detailed image of the patient’s retina. Thick retinal tissue is a sign that excess fluid has seeped into the retina.
Diabetic retinopathy treatment options
If you have already experienced permanent vision damage due to diabetic retinopathy, there are certain medications that may be able to help prevent further damage to your eyesight. There are also gentle laser treatments available that can assist in retaining your existing vision. A low vision specialist can recommend equipment that can magnify or augment your ability to see. If you have diabetic retinopathy, early treatment and frequent follow-up care can reduce your risk of blindness by up to 95 percent.
Anti-VEGF Medication
For this treatment, doctors inject anti-VEGF (vascular endothelial growth factor) medication like Lucentis, Avastin, and Eylea straight into the vitreous (clear liquid in the eye) to release the backup of fluids and stop new blood vessels from developing. These VEGF inhibitors need to be injected periodically for long-lasting results, but the good news is that they are successful in stabilizing vision in about 90% of diabetic retinopathy patients.
Focal Laser Treatment
Focal laser treatment, also known as photocoagulation, is a treatment that stops or slows blood from leaking into the eye by sealing faulty blood vessels. Pan-retinal photocoagulation is another laser treatment that uses heat energy to stop new, faulty blood vessels from developing in the eye.
Vitrectomy
For this surgery, an ophthalmologist drains the the vitreous from the eye to allow for easy removal of any blood and scar tissue that make vision worse in patients with diabetic retinopathy. The vitreous is then replaced with a clear synthetic fluid, which does not interfere with the normal functioning of the eye.

How can I prevent diabetic retinopathy?
Maintaining a healthy diet, exercising regularly, controlling your blood sugar, quitting smoking, watching your blood pressure, and receiving a yearly eye exam are all excellent ways to help reduce your risk of developing diabetic retinopathy.
Diabetic Retinopathy Costs
The cost of diabetic retinopathy treatment depends on which treatments are required to adequately address the problem and preserve your vision. Treatments are covered, at least in part, by most health insurance plans rather than vision insurance plans. Our team can help to review your coverage to provide an estimate of what benefits you are entitled to.
Contact Cascadia Eye
If you would like to learn more, or if you would like to schedule an appointment or consultation with our talented doctors at Cascadia Eye, please contact us today. Our entire team is committed to protecting and improving your vision and the health of your eyes. We are happy to answer any questions you might have!
In addition, join us on Facebook, Instagram or YouTube to ask your questions about eyes, exams, and our practice. We’d love to hear from you – and there might be a blog to address your questions in the future.


